Deep Learning for Prediction of AMD Progression
It is with great pleasure that we announce that Voxeleron’s work on deep learning for age-related macular degeneration (AMD) predictive analytics has been published in this February’s issue of Investigative Ophthalmology & Visual Science (IOVS).
More than 10 million people in the US have AMD, and globally it is the leading cause of vision loss for people over 50, responsible for 8.7% of blindness worldwide. Most people do not experience vision loss in the early, dry stages of AMD, but advanced, wet AMD can result in irreversible damage. Progression to wet AMD can occur without symptoms or measurable change, and doctors cannot predict when conversion may occur. Regular eye exams are used as an attempt to catch advanced AMD as early as possible, but this is expensive and impractical. In order to facilitate earlier intervention and treatment, better AMD prognostics are required, the topic of recent work by Voxeleron in collaboration with NIHR Moorfields BRC. We report on an artificial intelligence-based approach to predict the likelihood of a patient with dry AMD progressing to wet. The research, recently published, uses deep learning to look for subtle and diffuse patterns of change in 3D optical coherence tomography (OCT) images of a patient’s eye. Built around Orion, Voxeleron’s award-winning OCT analysis software, the work demonstrates strong performance in predicting which patients with dry AMD will convert, offering a novel solution to an extremely challenging clinical problem.
The paper can be found here and more information about the Orion software and our other products is available on our website.
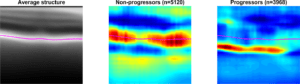
Figure 11 from the IOVS paper: Occlusion sensitivity analysis for progressors (right) and nonprogressors (middle). These images were derived by averaging the occlusion analysis outputs for all B-scans in their respective groups. The average structure for all B-scans is shown on the left, and the mean location of Bruch’s membrane in all scans is plotted in magenta. This analysis shows that, in particular, pixels around the RPE have the largest impact on the final score of the classifier for nonprogressors. It also suggests more sub-RPE or choroidal involvement for progressors.